Full textPDF
Full text
CASE REPORT
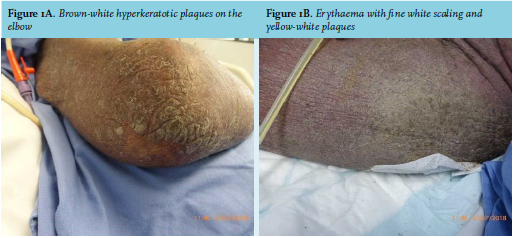
A 68-year-old male from Suriname was admitted to our intensive care unit (ICU) with progressive respiratory failure with a cavitating lung lesion. On admission, a de novo HIV infection with a CD4 count of 370 cells/µl and a viral load of 2.132.715 copies/ml was diagnosed. Cachexia was present (body mass index 16.9 kg/m2 ) with a blood pressure of 100/60 mmHg, pulse 124/ min and a temperature of 39.4°C. The patient was erythroderm and covered with brown-white plaques and profound white-yellowish scaling (figures 1A and B). His whole body, including his face and scalp was affected. His nails were discoloured, thickened and some were dystrophic. He continuously experienced pruritus, despite daily washing of his skin and twice daily applying Vaseline or indifferent ointment on his skin by nurses or family members. Severe scaling of the skin necessitated his bedsheets to be replaced frequently. A skin biopsy (from the elbow, see figure 1A) showed an orthokeratotic keratinizing epidermis, also slightly acantholytic thickening with an influx of lymphocytes. Immunohistochemical additional colouring did not identify herpes simplex, herpes zoster, or Borrelia. The intra-epidermal and peri-vascular lymphocytes were positive for marker CD3 and particularly CD4. Markers CD20 and CD30 were negative.
WHAT IS YOUR DIAGNOSIS?
See page 161 for the answer to this photo quiz.