Full textPDF
Full text
CASE REPORT 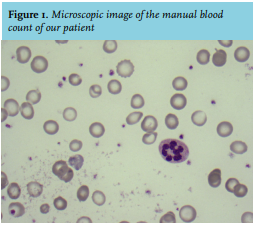
A 56-year old man of Egyptian descent was brought to our emergency room because of collapse preceded by subacute dyspnea and chest and back pain. His medical history included hypertension, hypercholesterolemia and two percutaneous coronary interventions six years and one year ago. We saw a pale man in distress, requiring 15 liters of oxygen via a non-rebreathing mask. He was clammy and had a sinus tachycardia of 100 beats/min with a blood pressure of 120/70 mmHg.
Blood gas analysis revealed lactate acidosis with pH 7.14, and a haemoglobin of 1.7 mmol/l. Therefore, two units of filtered erythrocytes were rapidly administered before cross-matching, with further transfusions given until a hemoglobin concentration of 5.0 mmol/l was achieved. There were no signs of external blood loss. A computed tomography scan of his thorax and abdomen did not reveal a bleeding site or other abnormalities. Meanwhile, further laboratory results indicated a mean corpuscular volume (MCV) of 66 fL, but no signs of hemolysis. The direct antiglobulin test did not demonstrate agglutination. A manual blood count was performed (see figure 1).
WHAT IS YOUR DIAGNOSIS?
See page 89 for the answer to this photo quiz.

