Full textPDF
Full text
CASE REPORT
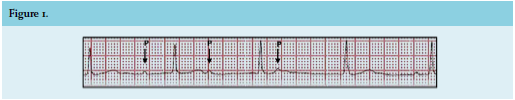
A 57-year-old female with a history of hypertension presented to the emergency department with extreme fatigue and dizziness. She had no complaints of chest pain or palpitations. Her current medication consisted of irbesartan and hydrochlorothiazide. She had a 7 pack-year history of smoking, drank alcohol occasionally, and she had no history of drug use. Her social pastimes included frequent walks in the woods. Family history for cardiovascular disease was negative. On physical examination the blood pressure was 126/65 mmHg, and she had a marked bradycardia with a heart rate of 47 beats/min. Other cardiac, pulmonary and neurological examinations were unremarkable. Routine laboratory tests showed a haemoglobin level of 8.0 mmol/l, leukocytes of 10.1 x 109/l, and a slightly elevated C-reactive protein of 21 mg/l. High-sensitive troponin was not elevated. There were no electrolyte abnormalities and thyroid studies showed no signs of hypothyroidism. Electrocardiography showed a third-degree AV block with nodal escape rhythm with a rate of 48 beats/min (figure 1). Chest X-ray was normal, transthoracic echocardiography did not show any structural abnormalities and a cardiac computed tomography scan showed no signs of obstructive coronary artery disease. Additional laboratory tests excluded the diagnoses of sarcoidosis, syphilis and amyloidosis.
WHAT IS YOUR DIAGNOSIS?
See page 419 for the answer to this photo quiz.