Full textPDF
Full text
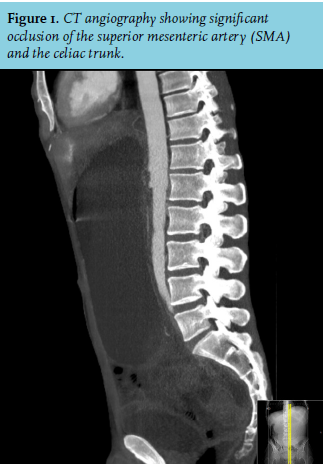
CASE REPORT
A 38-year-old patient was admitted to our hospital with signs of progressive abdominal angina, nausea, vomiting and cachexia, which had started four months earlier. His medical history reported seminoma 10 years before, for which he underwent orchiectomy followed by para-aortic radiotherapy (13 fractions of 26Gy). Within one year he presented with a local recurrence of the seminoma, which was successfully treated with chemotherapy. Further medical history included paranoid schizophrenia and drug abuse. There was no history of blood coagulation disorders or a family history of occlusive arterial disease.
The patient was referred to the psychiatric ward of our hospital by the psychiatrist from the mental health centre where he lived. The initial diagnosis was nonspecific abdominal pain combined with a delusional disorder, linked to his psychiatric and drug-related history. Thirty-eight days after presentation, a CT angiography was performed due to unsatisfactory clinical improvement, progressive abdominal pain and a high CRP (420 mg/l) (figure 1).
WHAT IS YOUR DIAGNOSIS?

